I wrote this last September not knowing it would get so much worse. I thought about this piece again as finally got COVID for the first time and as numbers for BA5 are rising. So far, ICU admissions and deaths have not risen as they have in the past. Myself along with all of us working in healthcare are crossing our fingers and hoping that remains true. Get Vaccinated! Get Boosted! JT
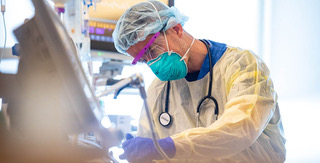
Walk with me through my ICU a few hours south of Chicago, the only one serving Coles County IL, with a population of just over fifty thousand. I want to offer you a window into my world to help give some clarity to yours. What you see here in our nine-bed unit I hope will help break through some of the mistrust and misinformation of these past eighteen months.
Gown on, gloves on, N95 mask: there’s a rhythm to donning the lifesaving barrier I wrap myself in every day, before I enter any room in my ICU.
First stop is ICU Bed 4. The patient is fifty, the same age as me. It’s hard to tell that, though, with his oxygen mask strapped so tight, distorting his face. He’s not vaccinated against COVID-19, but said he wishes he was now, a step away from needing a ventilator. Tune out the sound of air whistling through tubing, the undulating waveforms marching across the monitor and the mask, you can see his eyes, full of fear. It’s the fear patients feel when each breath they take is more labored than the last. The fear of isolation in a negative airflow room, intermittently interrupted by our team bursting in when patients turn a dusky blue. The fear that comes from knowing that there are things they left unsaid to those they love, but no longer have the luxury of enough air to say them.
Let’s move on to Bed 7. The patient, a woman, is sprawled out on the bed, face down, like a victim at a crime scene. We’re trying to open the lungs of this 45-year-old by rotating her again and again. This is her fifth day on a ventilator, the source of that harsh rhythmic noise from a breath so small being forced so quickly by a machine into her stiff and damaged lungs. That noise is the difference between life and death. But in the moments between the breaths, what you hear is the sound of loneliness. She lies face down, in a coma induced by the chemicals we give so that patients can tolerate the pain and discomfort of being on a ventilator. Her brainwaves have slowed, pain receptors blocked. There are tubes in her mouth, her trachea, her wrist, her neck, and her bladder keeping her alive. “Where is the family?” you might wonder. They come, but only for one hour a day. Visits are restricted due to the surging covid numbers in this community that is less than 40 percent vaccinated.
I’ve spent my fifteen years as a critical care doctor encouraging, even imploring, families to find ways to stay by the bedside 24/7. But because of COVID, I have been forced to change my tune. Now it’s just the drone of the ventilator to keep the patient in bed 7 company, 26 times a minute, 1560 times an hour and 37,440 times in a day.
We don’t have much time to see the patient in Bed 8. Or more accurately the patient in Bed 8 does not have much time. It is quiet in here. This patient’s ventilator has been removed and replaced by her son and sister sitting next to the bed. We make exceptions for more than one visitor sometimes – when a patient is dying. And what you are seeing here is the end of a person’s life. I can’t remember why she isn’t vaccinated. I hear so many different reasons that it’s hard to keep track. But it makes no difference now. The impermeable gowns and masks we wear cannot shield you from the sadness and regret in this room.
One more stop to see the patient in Bed 2. She is barely older than my 20-year-old daughter. Yes, she is so very still. That’s what being paralyzed looks like, when your ability to move is gone. Her instinct to fight against the machine forcing air into her inflamed and infected lungs is chemically cut off at the junction between nerve and muscle. We are begging, hoping, praying, cajoling her lungs to work just a little bit more. More oxygen so that her brain, her heart, her kidney and her liver won’t shut down. This patient needs a device called ECMO, a type of heart-lung bypass machine. My small hospital doesn’t have one, but bigger hospitals in bigger cities with heart surgeons and special perfusionists do. We’ve called surrounding hospitals in Chicago, Indiana and Missouri, but there are just too many young, sick patients and not enough ECMO units to go around. Desperation. That’s what fills this room. All we can do is wait and hope this patient gets the golden ticket, a transfer to another hospital, that just might allow her to fight for and live another day. Yet in this world of limited resources and zero-sum game, success is bittersweet. The extension of a buoy of hope for one means someone else is left to drown.
For doctors and nurses, breathing through a N95 mask all day adds to the heaviness that hovers everywhere in the ICU. Even the relief of peeling off the uncomfortable plastic gowns, we wear when we leave the ICU, is tempered by the chill of sweat covered skin. A covid filled ICU was never an easy place to be, but you can see and feel a difference in the staff this time. Last year the nurses, the doctors, the respiratory therapists, lab and x-ray techs, and all the units were one team, helping our community through a pandemic. Outside the hospital there was harsh political rhetoric mixed with lockdowns and mask mandates. But inside these walls we were one. One team, one voice.
What’s different now? Now we are a house divided, just like the rest of the country. On vaccines, on mandates, on culpability and personal responsibility. Our unity has been infiltrated and splintered and it makes the challenge of what lies in front of us more unbearable and daunting. Even in the ICU with a front row seat to the trauma COVID-19 has caused, some of my colleagues are still unvaccinated. I fear the upcoming Illinois and hospital vaccine mandates will drive a bigger wedge amongst a staff already under so much stress.
There is one more difficult space people need to understand that ICU doctors like me inhabit. In the physical rooms, you could see and hear and feel what is going on with patients. The other space is the place inside me where I try to contain my anger – at the unvaccinated and the purveyors of misleading information – and my fears that I’ve missed something, given up too early or pushed too hard. The fear that I won’t find an ECMO bed in time. It’s where I hold my frustration and desperation. Frustration about having more ICU patients than ICU beds and desperation about having to choose who gets one over another. It’s where I bear the weight of every family update I give, wishing I had something positive to share, but with COVID it would be a lie. With every phone call I make to a family, a little part of me breaks inside.
Last winter, nurses from other parts of the country swooped in to provide much needed respite and relief. Everyone is just too tired this time. So we are on our own. Waiting for this Delta surge to burn itself out. But that metaphor is not quite accurate. Embers and ash cannot really capture the tragedy of the dead left in covid’s wake.
Someday, I will have to reckon with my anger, my fear and desperation, but today is not that day. Today there are far too many people to treat, ventilators to modify, patients to prone. The infected just keep coming, with no end in sight. The unvaccinated are many. Our resources finite. But it is time for me to take a deep breath and keep moving forward. I have so many patients still to see, patients whose breath is being taken away.
Jeremy,
Our hearts break for what you must be enduring each day, but they are filled with admiration for your work (and the work of others like you).
Glad you are well, or getting there, and able to persevere. You are a wonder.
We send our love,
Joni and Pepper Dry
It’s good for all of us to read the truth. I hope it can influence someone to get the vaccine. How selfish can people be?
Jeremy, your vivid picture of the ICU is horrifying to read. I am so grateful for all that you do. You teach us all by letting us in.
Stay safe,
Dana Salzer
Dear Jeremy,
It is heartbreaking to know that so many people believe fake “science.” That you are able to keep on trying to save unvaccinated patients is a tribute to you as a doctor and human being. I couldn’t be prouder of you.
Hope you and Becky are feeling better.
Big Hugs,
Betty & all the Musburgers
Thank you for sharing your important and poignant perspective, friend. May you continue to find meaning and moments of peace and fulfillment in your work. May you get the support that you need every day, everywhere you turn. And may we all maintain our personal connections and mutual respect, despite our profound differences. Thank you for caring for the sickest among us, even when our sickness might have been prevented. Sending light and lightness through the dark and heavy!