by Jeremy | Apr 24, 2020 | Change, Medical, Medicine
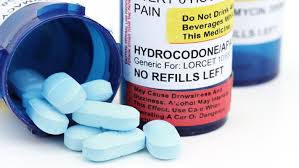
I’ve developed a formula to facilitate running after having surgery on my tongue: two-thirds medicinal, one-third mechanical. First, fifteen minutes prior to any run, take 3 tsp. of hydrocodone (definitely key to taking the edge off). Second, apply a generous amount...

by Jeremy | Apr 10, 2020 | Medical, Medicine, Transformation, Uncategorized
Artwork by https://lindsaymound.com/ The volume of COVID related news and information is overwhelming. There is 24/7 coverage on TV, Twitter and social media. Important medical information is being shared in real-time across the globe on lessons learned caring for...
by Jeremy | Apr 2, 2020 | Change, Medical, Transformation
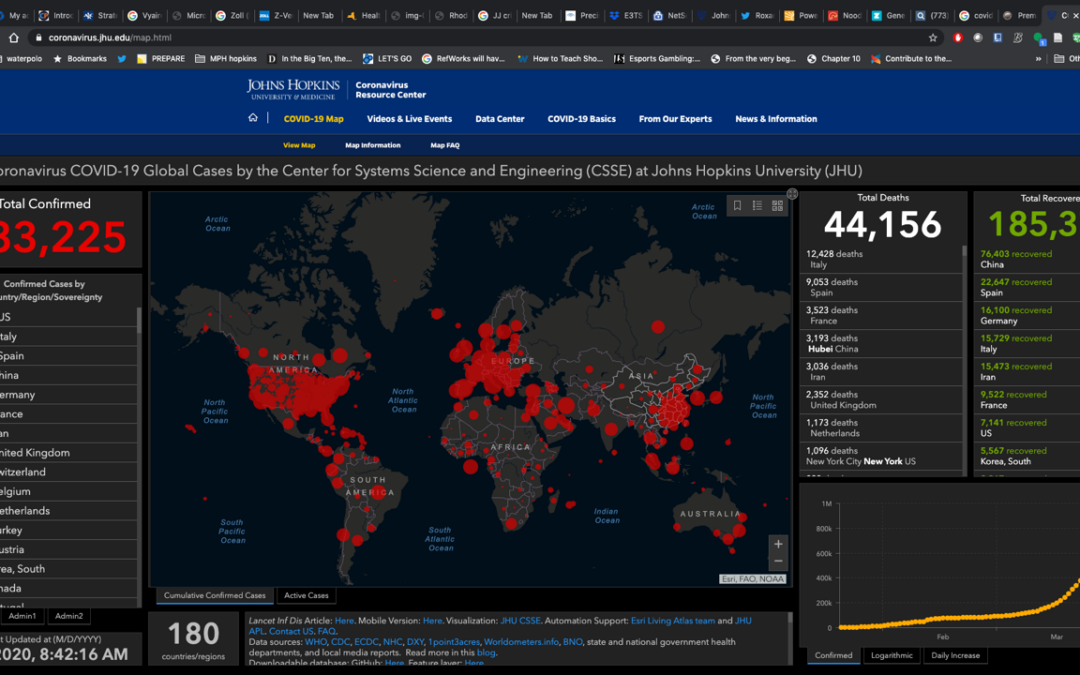
I’m an ICU doctor in the middle of a global pandemic. I am trained to manage ventilators and care for the critically ill. My city, along with others, is preparing for a surge of patients requiring hospitalization and intensive care. And I’m nowhere near a hospital....

by Jeremy Topin | Oct 21, 2019 | End of life, Medical
I am a runner. I run long to train for iron distance triathlons. I run for fun with friends in the cool early morning sun and for a hot venti americano after. I run to cope with the frustrations that comes with life and being a busy physician in today’s world. I am a...
by Jeremy Topin | Aug 28, 2018 | Balance, End of life, Medical, Medical Education, Parenting
It is my pleasure to introduce to the readers of Balance, Dr. Rebecca MacDonell-Yilmaz. Becky is a pediatrician out on the East coast who has not only just completed a fellowship in hospice and palliative care medicine, but has just embarked on her third board...

by Jeremy Topin | Feb 14, 2018 | Balance, End of life, Medical
This piece was written together with a friend and colleague Chadi Nabhan, an oncologist and current Chief Medical Officer at Cardinal Health. This was originally published here in The Oncologist. The crowd erupts with joy, champagne bottles pop open, and everyone...